Report says Illinois was ill-prepared for pandemic
By Peter Hancock Capitol News Illinois — July 8, 2020
Danny Chun, spokesman for the Illinois Health and Hospital Association, disagreed that hospitals weren’t prepared for the pandemic. “We’ve been drilling and doing exercises on pandemics before the pandemic hit.” The first person testing positive in Illinois was someone who came through O’Hare International Airport in January.
SPRINGFIELD – A new report from an Illinois think tank says the state was ill-prepared for the COVID-19 pandemic, primarily because of a pre-existing shortage of nurses, and that the pandemic has left state even more vulnerable in the event of another public health crisis.
The report, by the Illinois Economic Policy Institute, a nonprofit organization with strong ties to organized labor, also argues the state would be in a better position if nurses at more hospitals were unionized and if the state adopted a law requiring mandatory minimum nurse staffing levels, an idea that was proposed in the 2019 legislative session but was not adopted.
But while the Illinois Health and Hospital Association agrees there is a nursing shortage, it argues the lack of preparedness was more of a federal problem, and that the nursing shortage did not diminish the quality of care patients received.
It strongly opposes legislation requiring minimum nurse staffing levels at hospitals, and disputes any correlation between the quality of patient care and the presence of a nurses’ union in a hospital.
The report notes that even before the pandemic, Illinois had a shortage of about 20,000 nurses statewide and that the shortage will likely be exacerbated in the coming years because about half of the nurses practicing are older than 55.
“Even prior to the pandemic, more than 75 percent of registered nurses reported that insufficient staffing levels adversely affects their job satisfaction,” the report states, citing a national survey of nurses in 2019. “COVID-19 has the potential to exacerbate the nursing shortage if registered nurses feel even more overworked and stressed.”
The report examines patient care data from all 169 hospitals in Illinois, 14 of which are unionized and 155 of which are not. All but four of the unionized hospitals are in Cook County and include some of the largest health care facilities in the state.
Across all levels of care, it noted, nurses in unionized hospitals were able to spend more hours per day treating their patients. They also had lower turnover rates and lower vacancy rates for registered nurses.
The report does not draw specific connections to staffing levels, or union presence, and patient outcomes during the pandemic. Frank Manzo, the institute’s policy director, said it’s difficult to say with certainty the extent to which the nursing shortage contributed to the severity of the pandemic in Illinois.
“What we can say is that we could have had more infection prevention and control staff,” he said. “We could have had better turnover rates and retention rates for nurses and lower vacancy rates and that would have made us better prepared for the pandemic.”
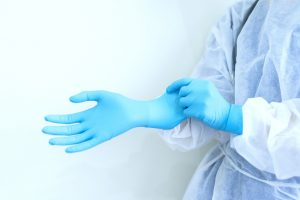
Illinois Health and Hospital Association and Illinois Economic Policy Institute agree there is a nursing shortage in the state. But, the IHHA says any lack of preparedness for the COVID-19 pandemic was more of a federal problem, and that the nursing shortage did not diminish the quality of care patients received. (University of Illinois Chicago photo)
Last year, Rep. Fred Crespo, D-Hoffman Estates, introduced House Bill 2604, which would have required hospitals to have at least one nurse for every four patients in medical-surgical units; one for every three patients in intermediate care; and one for every two patients in intensive care. The bill passed out of a House committee but was never voted on by the full House.
“If the legislation had been fully implemented, Illinois would have had between 17,500 and 19,100 more registered nurses — which would have eliminated the shortage of registered nurses,” the report states.
But Danny Chun, spokesman for the Illinois Health and Hospital Association, strongly disagreed that hospitals weren’t prepared for the pandemic.
“First of all, we’ve been drilling and doing exercises on pandemics before the pandemic hit,” Chun said during an interview. “Every hospital in the state, as you know, has an emergency preparedness plan for disasters of all kinds — mass shootings, traffic accidents, biochemical, biohazard, flu epidemics or pandemics. In the city of Chicago last year in the summer of 2019, Chicago hospitals did an exercise, a drill with the Chicago Department of Public Health on this exact issue — pandemics. And we were directly involved in a lot of the planning and discussions back in January, February, March where hospitals got ready for the pandemic.”
Chun said hospitals were directly involved in discussions with Gov. J.B. Pritzker’s administration in the early stages of the pandemic to plan mitigation efforts, including the decision to cancel or postpone nonemergency surgeries and procedures in order to free up hospital resources for COVID-19 patients.
“Look at the numbers. We flattened the curve,” Chun said, referring to hospitalization data from the Illinois Department of Public Health, which have shown a consistent downward trend since May in hospitalizations, intensive care admissions and ventilator usage by COVID-19 patients.
If there was any weakness in preparation, Chun said, it was with the federal government and its failure to maintain a national stockpile of personal protective equipment as well as open supply chains with China, where most PPE is manufactured.
Enacting a law requiring minimum staffing levels, Chun argued, would not solve the state’s nursing shortage and would likely harm many smaller hospitals as well as safety-net hospitals in urban areas that wouldn’t be able to meet the requirements.
“You have an existing shortage of at least 21,000 nurses in Illinois,” he said. “Simply requiring hospitals to have a certain number of nurses does not create new nurses. In and of itself, ratios don’t do anything.”
Chun argued that to address the nursing shortage, the state needs a multi-pronged strategy that includes more scholarships for nursing students, incentives to keep nurse educators in the workforce, and policies that would make it easier for nurses licensed in other states to practice in Illinois.



