Rural hospitals brace for surge of COVID-19
By Peter Hancock Capitol News Illinois — April 10, 2020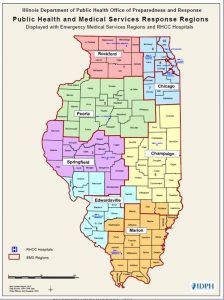
: The graph depicts Illinois’ public health and medical service response regions. (Credit: Illinois Department of Public Health)
SPRINGFIELD — Although the COVID-19 outbreak in Illinois so far has been mainly concentrated around the Chicago area, public health officials are bracing for a surge of cases in rural areas of downstate Illinois, including areas that already have shortages of hospital beds, health care providers and equipment.
“So, we’re keeping a close eye on that,” Illinois Department of Public Health Director Dr. Ngozi Ezike said April 8. “As we look right now, I think our hot spot is more northern Illinois … but we’re keeping an eye on all the beds, the ICUs, the ventilators and the availability of those, and we potentially, we’ll have to do some moving of things, but we are also looking at what the needs will be there.”
Despite health care shortages in some areas, Danny Chun, a spokesman for the Illinois Health and Hospital Association, said in an interview that most rural hospitals in Illinois should be well prepared for the surge, at least in terms of strategy.
“They are very prepared,” he said, citing two major trends in health care: industry consolidation over the past five to 10 years into health care “systems” that have the ability to share resources, and regional planning.
“A lot of small and rural hospitals, critical access hospitals, are now part of large systems, like OSF, HSHS, Carle, Southern Illinois Health,” Chun said.
“Then there’s an existing structure within the state of Illinois — they’re called Regional Health Care Coalitions,” he added. “There are 11 coalitions throughout the state covering every area of the state, including southern and central Illinois, where all the health care providers in that region get together in terms of emergency planning, pandemic planning, emergency exercises. That’s been in place for years.”
According to IDPH, each of those 11 regions has one main hospital designated as the coordinating center. For example, the Carle Foundation Hospital in Urbana serves as the coordinating center in the Champaign region, which covers 18 counties in east-central Illinois.
Anita Guffey, who serves as the emergency management coordinator and readiness and response coordinator for that region, was unavailable for an interview Wednesday due to the immediate demands on her time, as were her counterparts in other regions. But she issued a statement through a spokesperson saying the planning process for COVID-19 is not significantly different from the planning they go through for other emergencies.
“In this region we need to be prepared for tornadoes, blizzards, and even earthquake risk, in addition to pandemic planning,” she said. “Every incident is different, but we work on this at all times so when the time comes, we’re already familiar with each other.”
The one thing rural hospitals have not been prepared for, however, is the financial pressure resulting from dealing with the pandemic.
Chun said hospitals throughout the state postponed most outpatient and elective surgeries, a significant amount of their annual revenue, in order to free up space and medical staff for treating COVID-19 patients. They are also “ramping up” for the pandemic, he added.
“We are urging the state to take all the steps that they can to increase cash flow to hospitals, because as you know, they’re facing a double whammy,” he said. “…On the one hand, they’re losing money because they’re not doing elective surgeries and procedures, and then money’s going out the door because of the preparations for the virus.”
Chun noted that in March, the state comptroller’s office used inter-fund borrowing to increase its Medicaid payments to state hospitals, paying down about $200 million in past-due bills. But the comptroller’s office has already indicated that there will likely be additional payment delays in the coming months — the tax filing deadline was pushed back to July 15, and the economic slowdown brought on by the statewide stay-at-home order and closure of nonessential businesses.
The federal government temporarily increased its share of Medicaid funding by 6.2 percentage points, retroactive to Jan. 1. That reduces the state’s share of Medicaid costs, freeing up general revenue funds for other purposes.
The biggest boost hospitals will see in the near term will come from the $2.2 trillion federal recovery package Congress recently passed, known as the Coronavirus Aid, Relief and Economic Security Act.
Chun said that package includes more than $100 billion for hospitals across the country to help offset the cost of responding to the pandemic, including some automatic funding increases and some reimbursement programs that hospitals must apply for.
But even with that, Chun said, hospitals across the country will need additional assistance.
“We are now preparing to ask the Illinois General Assembly for help on the state level with Medicaid funding for our hospitals,” he said. “So whenever the legislature finally returns — you know, maybe in May, maybe in June — we will be asking the General Assembly for help for our hospitals.”
phancock@capitolnewsillinois.com







