State public health officials monitoring suspected Monkeypox Cases
June 16, 2022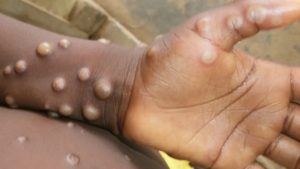
Monkeypox is a rare but potentially serious viral illness that typically begins with flu-like illness and swelling of the lymph nodes and progresses to a rash on the face and body. (W.H.O. photo)
The Illinois Department of Public Health (IDPH) is continuing to work with the CDC and local public health officials to investigate suspected cases of monkeypox virus in Illinois. As of June 16, IDPH is reporting 10 Illinois cases, eight that have been confirmed by CDC, including nine in Chicago and one in DuPage.
While Monkeypox is a rare disease and does not spread easily between people without close contact, IDPH officials urge the general public to be aware of the small but growing number of cases that have been identified. The threat of monkeypox to the general U.S. population remains low.
IDPH staff are working with the Chicago Department of Public Health, the DuPage County Health Department and healthcare providers to identify individuals who may have been in contact with the patients while they were infectious.
In the United States, the CDC is reporting 84 cases reported in 19 states and the District of Columbia. Most of the infected individuals have reported only mild symptoms, and none have died.
The CDC has issued guidance for the general public on how to stay safe from monkeypox while attending festivals, parades and other summer events where close, personal, skin-to-skin contact is likely to occur. If individuals feel sick or have rashes or sores, public health officials recommend they not attend gatherings, and visit a healthcare provider as soon as possible.
The CDC is tracking multiple clusters of monkeypox that have been reported within recent weeks in the U.S. and many countries that don’t normally report monkeypox.
These cases include individuals who self-identify as men who have sex with men. CDC is urging healthcare providers in the U.S. to be alert for patients who have rash illnesses consistent with monkeypox, regardless of whether they have travel or specific risk factors for monkeypox.
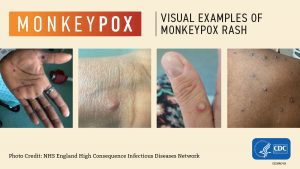 Anyone, regardless of sexual orientation, can spread monkeypox through contact with body fluids, monkeypox sores, or shared items (such as clothing and bedding) that have been contaminated with fluids or sores of a person with monkeypox. Monkeypox virus can also spread between people through respiratory droplets typically in a close setting, such as the same household or a healthcare setting. Common household disinfectants can kill the monkeypox virus.
Anyone, regardless of sexual orientation, can spread monkeypox through contact with body fluids, monkeypox sores, or shared items (such as clothing and bedding) that have been contaminated with fluids or sores of a person with monkeypox. Monkeypox virus can also spread between people through respiratory droplets typically in a close setting, such as the same household or a healthcare setting. Common household disinfectants can kill the monkeypox virus.
Monkeypox is a rare but potentially serious viral illness that typically begins with flu-like illness and swelling of the lymph nodes and progresses to a rash on the face and body. Most infections last two-to-four weeks. In parts of central and west Africa where monkeypox occurs, people can be exposed through bites or scratches from rodents and small mammals, preparing wild game, or having contact with an infected animal or possibly animal products.
The virus does not spread easily between people; transmission can occur through contact with body fluids, monkeypox sores, items that have been contaminated with fluids or sores (clothing, bedding, etc.), or through respiratory droplets following prolonged face-to-face contact.
What people should do:
- People who may have symptoms of monkeypox, particularly men who report sex with other men, and those who have close contact with them, should be aware of any unusual rashes or lesions and contact their healthcare provider for a risk assessment.
What healthcare providers should do:
- If healthcare providers identify patients with a rash that looks like monkeypox, consider monkeypox, regardless of whether the patient has a travel history to central or west African countries.
- Do not limit concerns to men who report having sex with other men. Those who have any sort of close personal contact with people with monkeypox could potentially also be at risk for the disease.
- Some patients have had genital lesions and the rash may be hard to distinguish from syphilis, herpes simplex virus (HSV) infection, chancroid, varicella zoster, and other more common infections.
- Isolate any patients suspected of having monkeypox in a negative pressure room, and ensure staff understand the importance of wearing appropriate personal protective equipment (PPE) and that they wear it each time they are near suspected cases.
- Consult the state health department or CDC’s monkeypox call center through the CDC Emergency Operations Center (770-488-7100) as soon as monkeypox is suspected.
For more information about the current cases of monkeypox in the U.S., go to: https://www.cdc.gov/poxvirus/monkeypox/outbreak/us-outbreaks.html







