Living with Alzheimer’s: Making holidays supportive and happy for all
By Elise Zwicky For Chronicle Media — December 9, 2018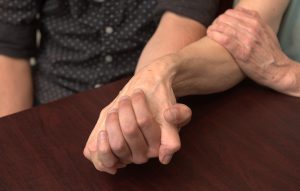
The holidays can be challenging and stressful for caregivers providing care for a loved one living with Alzheimer’s. With planning, communication and adjusted expectations, however, they can still be happy and memorable occasions for families. (Photo courtesy of the Alzheimer’s Association Illinois Chapter)
When Barry Burns’ mother and sister developed dementia, the family tradition of cooking the holiday meals shifted to others. Now that the Peoria man’s wife, Vicki, is in the early stages of Alzheimer’s, the family is facing similar decisions.
“We haven’t (hosted the holidays) in a couple of years, but I think she’d have a little harder time remembering the ingredients if she did all the cooking like she used to,” Burns said of his wife of 51 years. “Last year our daughter was here, and she pretty much did everything.”
While often joyous, the holidays can be stressful for anyone, but particularly for the 590,000 caregivers like Burns who are providing care for the 220,000 people living with Alzheimer’s in Illinois.
“During the holidays, we’re extra busy, there are extra expectations and you’re dealing a lot more with family that maybe hasn’t been around as much, so they may not really understand what’s happening,” said Daryl Carlson, manager of education and outreach in the Peoria office of the Alzheimer’s Association Illinois Chapter.
Melissa Tucker, director of helpline and support services in the Alzheimer’s Association’s Chicago office, added, “People feel pressure to make the holiday a perfect experience. And if you’re the person who’s providing full-time care for somebody with dementia, you’re probably not the best person to be completely responsible for preparing the holiday dinner or doing all the gift-giving. So you have to be really realistic about what you’re going to be able to take on.”
Both experts agree, however, that the holidays can still be happy and memorable for everyone with some advanced planning and adjusted expectations.
One tip is to be open with family and friends about what to expect before they arrive for a visit.
“Other people have expectations, too, and they may not really understand what’s happening right now,” Carlson said. “So consider giving people a heads-up maybe by sending a pre-Christmas letter to those you want to make plans with to say, ‘Hey this is where they’re at right now.’ Just try to communicate really well with everybody.”
Burns agreed, noting, “I think the ones it would be most stressful for during holiday times are the ones that are in denial and want to try to hide it. It’s better to let people know and to talk about it and face it and get help.”

Families and friends of people living with Alzheimer’s may be unsure of how to involve their loved one in holiday activities without overwhelming them or others, but the Alzheimer’s Association offers tips on how to modify family traditions to ease some of the stress. (Photo courtesy of the Alzheimer’s Association Illinois Chapter)
Having that conversation with family members ahead of time can be especially important if the family lives out of town and hasn’t seen the person with dementia for some time, Tucker said.
“That’s one more of those family conversations that can be very difficult,” she noted. “But it’s important to talk about how things are different and the need to start some new traditions or scale back the old ones and the importance of delegating some things.”
Carlson also recommended talking to the grandchildren ahead of time to explain that grandma or grandpa isn’t able to remember as well and might get confused.
“Really encourage the kids not to quiz them,” he said. “That’s very much a kid thing to do to ask: ‘Do you remember me? Do you remember my name?’ Even some adults need to be reminded not to ask those kinds of questions.”
Another tip is to take time to experiment with new traditions that might be less stressful or a better fit with caregiving responsibilities, such as turning a traditional holiday dinner into a holiday lunch if evening confusion and agitation are a problem.
Carlson said it’s also important to include the person with dementia as much as possible.
“This disease affects their mind, but they still have the same emotional needs as everyone else, though their ability to express that is diminished” he said.
Depending on abilities and preferences and what stage the person is at in the progressive disease, the patient might still enjoy activities such as packing cookies in tins or helping to wrap gifts.
“Make sure it’s something they have enjoyed in the past and something they like to do,” Carlson said. “Then make sure it’s a size that they can handle with just two or three steps if they’re early in the disease or just one step if they’re further along.”
Tucker added, “People are sometimes sad about the changes and want to recreate the way things used to be, but you may have to process that and let that go. You have to be realistic about what your loved one is going to enjoy.”

Caregivers of a person with Alzheimer’s can cope with holiday stress by adjusting their expectations and looking for ways to involve their loved one in meaningful activities they still can enjoy while still watching for cues that they might be getting overwhelmed. (Photo courtesy of the Alzheimer’s Association Illinois Chapter)
Despite the best-laid plans, Carlson said caregivers should be prepared for their loved one to become overstimulated during holiday events.
“Bring a bag with things you know they like to do that’s simple and calms them down,” he said, noting that might mean having a device loaded with quiet music they can listen to by themselves or having a fidget quilt they can hold.
“Be aware and look for the signs. For each person it’s different. Whether they’re fidgeting or pacing or if they seem to start getting short with people, intervene early and make sure to pull them off to someplace less stimulating to help them calm down,” he said. “Sometimes they might even be staring at a wall, kind of shutting down.”
During the holidays or anytime, help is available by calling the Alzheimer’s Association Helpline at 800-272-3900, which is staffed 24 hours a day, seven days a week.
“The Helpline fields a huge variety of questions,” Tucker said. “You can speak to a counselor or social worker, and we have people who speak Spanish, as well as an interpreter line so we can take calls in all different kinds of languages.”
More help and information for caregivers can also be found at www.alz.org/help-support.
Tips for navigating holiday travel with loved one with Alzheimer’s
As people conduct their holiday travel this year, planning and completing a long-distance trip can be very stressful for the more than 220,000 Illinois residents currently living with Alzheimer’s and their families.
While the symptoms of this progressive brain disease can sometimes make travel more difficult, it doesn’t mean families can’t travel with a loved one with dementia and participate in holiday festivities.
The Alzheimer’s Association Illinois Chapter offers several easy tips to help ensure a safe and smooth trip when traveling with a person living with dementia.
- Stick with the familiar: Travel to known destinations. Try to visit places that are familiar.
- Be prepared: Create an itinerary that includes details. Give copies to family members or friends. Keep a copy with you.
- Pick the right time: Travel during the time of day that is best for the person with Alzheimer’s
- Avoid layovers: If unavoidable, ask about airport escort services.
- Ask for help: For example, request airline personnel to help you navigate through the airport.
- Ensure a Safe Return: Changes in environment can trigger wandering.
- Find local support: Before you go, contact the Alzheimer’s Association chapter at your destination.
More tips and information are also available at org/travel.







